Blood NfL Levels May Be Useful Marker of Polyneuropathy and Its Severity
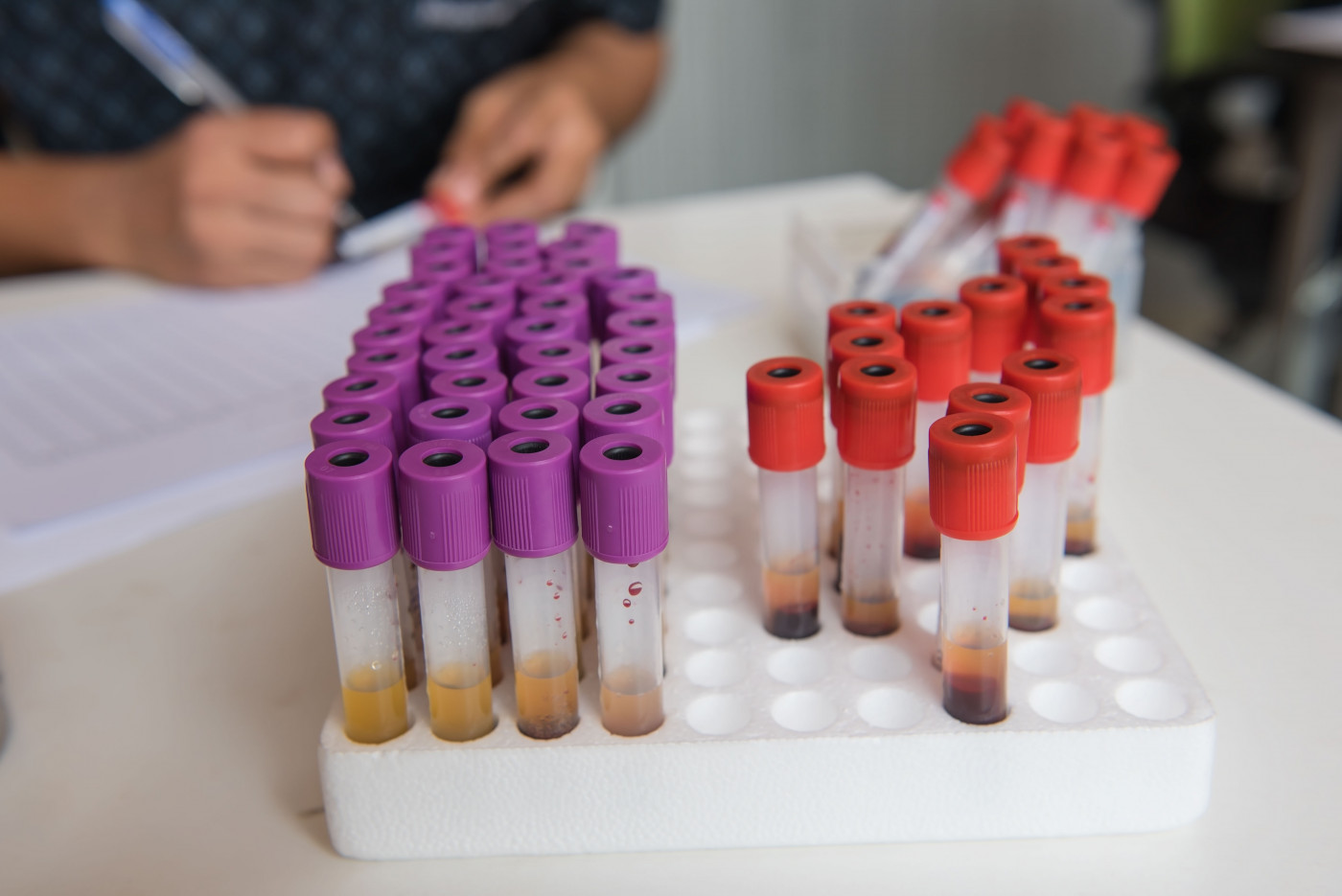
Blood levels of neurofilament light chain (NfL) — a protein commonly used as a marker of nerve cell death in neurodegenerative disorders — associate with the severity of peripheral nerve damage (polyneuropathy) in people with familial amyloid polyneuropathy (FAP), a study reports.
In fact, NfL seems to be a promising biomarker of polyneuropathy, both for people with FAP and those with other forms of amyloidosis, its researchers suggest.
The study, “Neurofilament light chain, a biomarker for polyneuropathy in systemic amyloidosis,” was published in Amyloid.
Amyloidosis comprises several disorders resulting from the accumulation of misfolded proteins within different organs, interfering with their normal function.
Amyloid light chain (AL) amyloidosis and hereditary transthyretin-related (ATTRv) amyloidosis, also known as FAP, are two forms of systemic amyloidosis. While AL amyloidosis is triggered by the buildup of small portions of antibodies called light chains, FAP is caused by the accumulation of a misfolded protein called transthyretin.
In both forms of amyloidosis, peripheral nerves — those that control movement and sensation in the limbs — are often damaged by the buildup of these harmful protein aggregates. This can lead to polyneuropathy, a condition characterized by a loss of sensation, numbness, tingling, and pain in the extremities.
“Detecting PNP [polyneuropathy] at an early stage is important for diagnosing new patients and is crucial for prognosis and choice of treatment,” the researchers wrote.
However, current techniques to detect polyneuropathy are burdensome, at least to some degree, and have limited sensitivity when it comes to spotting early signs of nerve damage. For this reason, “there is a clear clinical need for an easily applicable serum biomarker for both the early detection and follow-up of PNP in systemic amyloidosis.”
Researchers at University Medical Center Groningen, in the Netherlands, and colleagues investigated if NfL, a key protein component of neurons that is released into the bloodstream when nerve cells are damaged, might be useful as a biomarker of polyneuropathy in patients with AL amyloidosis and FAP.
To measure NfL serum levels, researchers collected blood samples from patients with both types of amyloidosis, as well as from a group of healthy people serving as controls. Of note, serum is the portion of blood that can be obtained once all blood cells are removed.
A total of 20 patients with AL amyloidosis, including 10 with and 10 without polyneuropathy, 15 people with FAP and polyneuropathy, and 15 asymptomatic carriers for the TTR mutation associated with FAP, were included in the analyses.
Of the 25 controls, 10 were matched in age and sex to the AL amyloidosis group, and 15 were matched to the FAP group.
Compared to age- and sex-matched controls, patients with AL amyloidosis had significantly higher levels of NfL in their blood.
However, among those with AL amyloidosis, NfL levels were found to be 6.6 times higher in the subset of patients who also had polyneuropathy, compared with those who did not have this condition.
NfL levels were also higher in patients with FAP and polyneuropathy, compared with asymptomatic mutation carriers (9.6 times higher) and controls (7.5 times higher).
Within the subgroup of FAP patients with polyneuropathy, the researchers also found that NfL levels tended to be higher among those with walking difficulties (PND score higher than I) than among those with only sensory impairments and at an earlier stage of polyneuropathy (PND score of I).
No significant differences in NfL levels were observed between asymptomatic TTR mutations carriers and healthy individuals.
“NfL is a promising biomarker for the detection of PNP, not only in ATTRv but also in AL amyloidosis. Serum NfL is able to detect PNP in an early symptomatic disease stage and correlates with severity of PNP,” the investigators wrote.
“Longitudinal studies are necessary to evaluate whether NfL is a sensitive marker for the detection of both PNP and small fibre neuropathy early in an asymptomatic stage in AL and ATTRv amyloidosis,” they concluded.






