Unique Set of Predictors to Distinguish Familial Amyloid Polyneuropathy Identified in Analysis
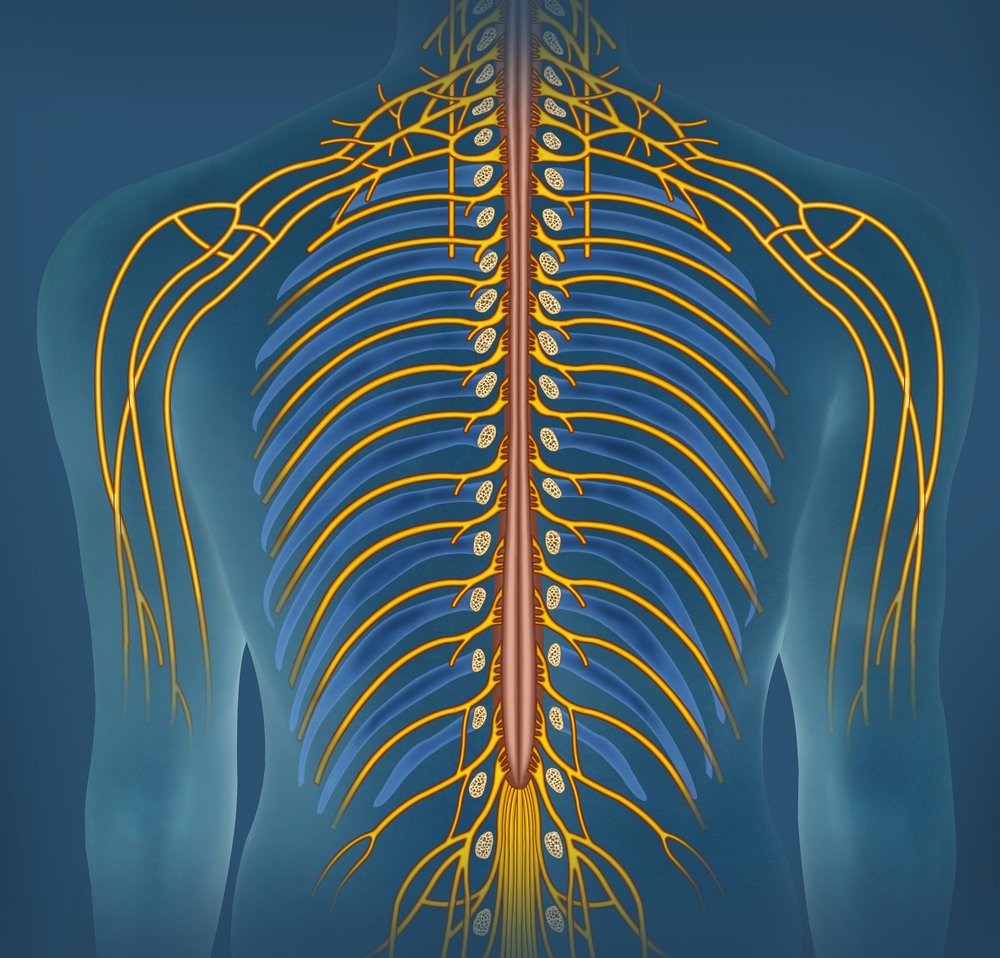
A series of potential predictors for identifying patients with familial amyloid polyneuropathy (FAP) and distinguishing it from other diseases with similar symptoms, namely chronic inflammatory demyelinating polyneuropathy (CIDP), were recently found through a retrospective analysis.
The study, “Transthyretin amyloid polyneuropathies mimicking a demyelinating polyneuropathy,” was published in the journal Neurology.
Familial amyloid polyneuropathies can have overlapping symptoms with CIDP, a neurological disorder characterized by progressive weakness and impaired sensory function in the legs and arms. In fact, approximately 61 percent of FAP cases are initially diagnosed as CIDP.
In this analysis, researchers compared a group of patients with demyelinating FAP with CIDP patients and those with POEMS syndrome. POEMS is short for polyneuropathy, organomegaly, endocrinopathy, monoclonal protein, and skin changes, a rare demyelinating disorder that damages the nerves and affects several parts of the body.
Researchers investigated the clinical and electric activity-related symptoms of FAP patients who also fulfilled the criteria for a CIDP diagnosis at an initial evaluation.
They evaluated a group of 194 FAP patients — 110 patients of Portuguese origin had early-onset FAPs, and 84 of French ancestry had late-onset FAPs. Of the French ancestry cases, 13, or 15%, fulfilled the criteria for demyelinating FAP.
A comparison of the clinical manifestations between all three groups showed that patients with demyelinating FAP had a set of more frequent symptoms than those in the CIDP and POEMS groups.
These signs that could distinguish demyelinating FAP patients were: neuropathic pain (the outcome of damage or injury to the nerve cells from the peripheral and central nervous system); dysautonomia (failure of the autonomic nervous system, the one responsible for controlling body functions, like breathing and heartbeat); small nerve fiber sensory loss above the wrist; and weakness in the arms.
“Our study identified several clinical and electrophysiologic markers that should alert to possible FAP in patients with suspected CIDP,” the researchers wrote.
They also noted that none of these predictors are currently part of the 2010 European Federation of Neurological Societies/ Peripheral Nerve Society (EFNS/PNS) criteria, which is used as a guide to help identify CIDP.
Overall, “our study identified a number of reliable distinctive features of dFAPs [demyelinating FAPs],” they wrote.
“These could be used as red flags by physicians to prompt TTR genetic testing [the genetic proof for TTR-FAP], enabling earlier diagnosis of FAP and initiation of specific treatments, thus improving the clinical course of the neuropathy and patient survival,” the study concluded.