Amyloid Deposits in Skin Samples Could Be Alternative to Biopsy in Diagnosing FAP, Study Suggests
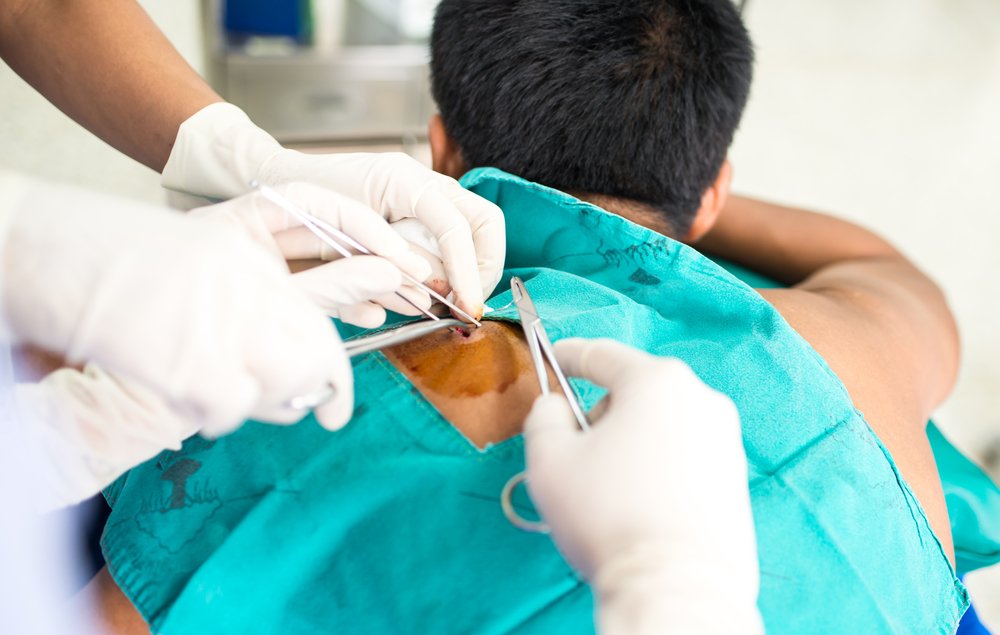
A skin sample might aid physicians in diagnosing patients with familial amyloid polyneuropathy (FAP) caused by mutations in the TTR gene, according to a study that showed that amyloid deposits, which cause nerve disease in these patients, are also present in the skin.
In addition to sparing patients more invasive nerve biopsies, measuring amyloid burden in the skin may serve as a marker of treatment effectiveness in future clinical trials in FAP, the researchers at Johns Hopkins University argue.
Their study, “Cutaneous Nerve Biomarkers in Transthyretin Familial Amyloid Polyneuropathy,” was published in the journal Annals of Neurology.
While typical FAP symptoms, such as tingling and prickly burning sensations in the legs, might indicate disease onset in a person with a family history of FAP, those without such a history are often misdiagnosed or diagnosed late because the condition can be difficult to correctly identify.
Studies show that sampling the sural nerve in the calf might show changes typically linked to the disease — such as amyloid deposits surrounding nerve fibers and a reduction of smaller nerve fibers.
But these changes are known to occur in a patchy distribution, so that a biopsy could miss information that might lead to a diagnosis.
As a skin sample is a simpler and less invasive procedure, the research team recruited a range of patients to test if changes in amyloid are also present there.
The study included 20 people with TTR-linked FAP, 10 patients with TTR mutations but no nerve disease, 20 with diabetic neuropathy, two patients with amyloid light-chain (AL) amyloidosis, and 20 healthy controls.
Analyses showed that in FAP patients, compared to controls, the density of nerve fibers was markedly lower in the epidermal (outer) layer of the skin and in the sweat glands, as well as in the nerves of muscles attached to hair follicles on the skin.
Those with TTR mutations but no nerve disease had nerve fiber densities that were superior to FAP patients but inferior to healthy controls. Lower nerve fiber densities were linked to patients’ level of impairment.
The researchers also detected amyloid deposits in the skin of 70 percent of these FAP patients and 20 percent of people with mutations but no disease. The amount of amyloid in a patient’s skin correlated with the various nerve fiber density measurements, as well as the level of impairment.
The two people with AL-amyloidosis also had amyloid in their skin, while those with diabetic neuropathy had no amyloid present.
These findings suggest that the levels of amyloid, along with nerve fiber densities in the skin, could allow physicians to discriminate between FAP and other types of neuropathies, and aid in setting an early diagnosis.